When we think of potentially harmful exposures in the workplace we often think about chemical hazards, but there are also physical elements like ergonomic hazards, noise, vibration, radiation, cold and heat that can injure or even kill us.
Every day, millions of workers are exposed to high levels of heat in their workplaces and this exposure can be a matter of life and death. Even though illness from exposure to heat is preventable, every year, thousands become sick from occupational heat stress, and in some cases, die from this exposure.
Global warming is affecting local environmental factors which have caused external temperatures to reach daily highs in recent years. These factors may amplify already hot outdoor or indoor conditions, creating an unsafe work environment for the workers exposed to this hazard.
WHAT IS HEAT STRESS?
Heat stress is an environmental and occupational hazard, resulting from physical activity in hot or humid environments capturing a spectrum of heat-related illnesses, including heat stroke, which can lead to death. Just like you can’t let a car engine overheat or it shuts down, you don’t want your body to get too hot. Working in the heat puts stress on our body’s cooling system. High temperatures and high humidity, stress the body’s ability to cool itself and heat illness can become a deadly concern.
WHAT AFFECTS HEAT STRESS?
There are four environmental factors that affect the amount of stress a worker faces in a hot work
environment:
- temperature
- humidity
- radiant heat (such as from the sun or a furnace) and
- air velocity.
The level of stress the individual faces is highly dependent a number of personal characteristics such as:
- age
- weight
- fitness
- pre-existing medical conditions such as diabetes, kidney and heart problems, pregnancy, being overweight
- acclimatization to the heat
- alcohol or drug use.
If you have any of these dependent factors you should talk to your doctor about the work you do, and find out whether there are any special precautions you need to take to protect yourself.
WHO IS AFFECTED BY HEAT STRESS?
Many Unifor members spend at least some part of their working lives exposed to a hot working environment.
These include workers in workplaces such as:
- foundries, boiler rooms
- oil and gas drilling sites
- oil refineries
- mines
- construction sites
- demolition projects
- power plants
- paper mills
- warehouses
- casting operations
- steel mills
- vehicle assembly
- components plants
- laundries
- kitchens
- bakeries
- utilities
- and more
BE AWARE, ALERT AND ACTIVE
Heat stress can often affect you before you even realize it, so it’s important to be very aware of the signs.
Tragically, there have been incidents where workers have seemed fine during a work shift and a couple of hours later were found having seizures or were found unconscious. Specialty work (like in a confined
space), especially with heat-generating equipment or appliances, can quickly render workers exhausted and overheated. Workers wearing protective gear or equipment are at an even higher risk for heat-related issues, given that protective gear can trap heat next to the body.
Exposure to extreme heat conditions can result in heat stroke, heat exhaustion, heat cramps, or heat rashes. This exposure can also increase the risk of injuries in workers as it may result in sweaty palms, fogged-up safety glasses, and dizziness. Burns can also occur as a result of accidental contact with hot surfaces or steam. Hazardous heat exposure can occur indoors or outdoors, and can occur during any season if the conditions are right, not only during heat waves.
THE PRECAUTIONARY PRINCIPLE AND HEAT STRESS
After the SARS inquiry in 2003, Ontario Commissioner Justice Archie Campbell wrote that “we cannot wait for scientific certainty before we take reasonable steps to reduce risk.”
Campbell’s report identified the precautionary principle as an approach for protecting workers in circumstances of scientific uncertainty. This reflects the need to take prudent action in the face of potentially serious hazards without having to wait for complete scientific proof that a course of action is necessary.
In other words, we do not need to be certain that we are correct when we take action to protect ourselves when dealing with an occupational hazard.
We must use the Precautionary Principle whenever we encounter uncharted or new workplace hazards.
HOW OUR BODIES COPE WITH HEAT
In a warm environment, especially when physically active, the human body relies on its ability to get rid of excess heat (i.e., heat dissipation) to maintain a healthy internal body temperature. Heat dissipation happens naturally through sweating and increased blood flow to the skin.
However, if the muscles are being used for physical labour, less blood is available to flow to the skin and release the heat. Sweating is effective only if the environmental humidity level is low enough to permit evaporation and if the fluids and salt lost are adequately replaced.
Workers over 40 years old should be more even more careful because of a reduced ability to sweat. If the body cannot dispose of excess heat, it will store it. When this happens, the body’s core temperature rises and the heart rate increases.
Workers cool down faster if the external (environmental) heat and physical activity (metabolic heat) are reduced. If heat dissipation does not happen fast enough, the internal body temperature will keep rising and the worker may experience a number of symptoms including thirst, irritability, a rash, cramping, heat exhaustion, or even heat stroke. Heat stroke is a very severe heat-related illness.
Workers suffering from heat stroke experience mental dysfunction such as unconsciousness, confusion, disorientation, slurred speech or even death. This calls for immediate and critical response.
Cool the victim immediately and call 911!
When heat stroke doesn’t kill immediately, it can shut down major body organs causing acute heart, liver, kidney and muscle damage, nervous system problems, and blood disorders. Workers suffering from heat exhaustion are at greater risk for accidents, since they are less alert and can be confused.
LOOK OUT FOR THESE CONDITIONS
People react differently, so you may have just a few of these symptoms, or most of them:
- Headache
- Nausea, vomiting
- Feeling faint
- Fainting
- Dizziness
- Weakness
- Irritability
- Confusion
- Thirst
- Heavy sweating
- Elevated body temperature
- Decreased urine output
HEAT STRESS HAZARDS - SIGNS AND SYMPTOMS
Heat Rash, also known as “prickly heat,” may occur in a hot and humid environment when sweat is not easily removed from the surface of the skin by evaporation. When extensive or complicated by infection, heat rash can be so uncomfortable that it inhibits sleep, and impedes a worker’s performance or even results in temporary or total disability. It can be prevented by resting in a cool place and allowing skin to dry.
Heat Cramps are painful spasms of the muscles, are caused when a worker drinks large quantities of water but fails to replace their body’s salt loss. Tired muscles - those used for performing the work - are usually the ones susceptible to cramps. Cramps may also occur during or after working hours and may be relieved by taking liquids by mouth or saline solutions intravenously for quicker relief, if medically determined to be required.
Heat Exhaustion results from the loss of fluid through sweating when a worker has not replaced enough fluids by drinking or taken in enough salt or both.
The worker with heat exhaustion still sweats but experiences extreme weakness, fatigue, giddiness, nausea or headache. The skin is clammy and moist, the complexion may be pale or flushed and the body temperature is normal or slightly higher.
Treatment is usually simple. The victim should rest in a cool place and drink an electrolyte solution (a beverage used by athletes to quickly restore potassium, calcium and magnesium salts). Severe cases involving victims who vomit or lose consciousness may require longer treatment under medical supervision.
Heat Fatigue resulting from prolonged heat exposure, causes a decline in coordination, alertness, and performance. With so much blood going to the periphery of the body, less is available for muscles. Strength drops and fatigue kicks in sooner that otherwise. Accidents are more likely to happen. For example, accident rates for heavy machine operators double when they work in hot environments.
Fainting or “heat syncope” may be a problem for the worker unacclimatized to a hot environment by standing still in heat. Victims usually recover quickly after a brief period of lying down. Moving around, rather than standing still, will usually reduce the possibility of fainting.
Heat Stroke, the most serious health problem for workers in hot environment, is caused by the failure of the body’s internal mechanism to regulate its core temperature. Sweating stops and the body can no longer rid itself of excess heat.
Signs and symptoms include:
- mental confusion, delirium, loss of consciousness,
- convulsions or coma.
- a body temperature of 41 C (106 F) or higher.
- hot dry skin which may be red, spotty or bluish.
Victims of heat stroke will die unless treated promptly. While waiting for medical help, the victim must be removed to a cool area and his or her clothing soaked with cool water. He or she should be fanned vigorously to increase cooling.
Prompt first aid can prevent permanent injury to the brain and other vital organs.
SUSCEPTIBILITY TO OTHER TOXINS
Heat stress can aggravate the effect of other toxins. Dehydration and loss of minerals through sweat decreases the body’s ability to detoxify chemicals. Because the circulatory system is under strain, other hazards increase. Carbon monoxide, which reduces oxygen supply to the tissues, is of particular concern. Because of this, standards for other substances should be adjusted downward for the workers, working in a hot environment.
FIRST AID
Treat a worker suffering from heat exhaustion by:
- Stopping activity
- Moving the person out of the heat and into a shady or air-conditioned place
- Laying the person down and elevate the legs and feet slightly
- Removing tight or heavy clothing
- Having the person drink cool water or other non-alcoholic beverage without caffeine
- Cooling the worker with cold compresses or have the worker wash head, face, armpits, and neck with cold water
- Seeking medical treatment
Call 911 or your local emergency number if the person’s condition deteriorates, especially if the worker experiences:
- Fainting
- Agitation
- Confusion
- Seizures
- Inability to drink
- A core body temperature of 40 C (104 F) (heatstroke)
ACCLIMITIZATION
Acclimatization is the result of beneficial physiological adaptations (like increased sweating efficiency) that occur after gradual increased exposure to a hot environment. This process of building tolerance is called heat acclimatization. Not being used to working in the heat can be a major problem. Many workers who die from heat stroke are often in their first few days on the job or were working during a heat wave. If you haven’t worked in hot weather for a week or more, your body needs time to adjust. You will need to take more breaks and not do too much strenuous work during your first weeks on the job.
EMPLOYER RESPONSIBILITIES
The old proverb that “an ounce of prevention is worth a pound of cure” really applies to heat stress and worker protection. Employers have a legal duty to take every precaution reasonable in the circumstances for the protection of a worker. This includes developing policies and procedures to protect workers in hot environments due to hot processes or hot weather (or both). Employers must provide training to workers so they understand what heat stress is, how it affects their health and safety, and how it can be prevented. For compliance purposes, the respective Ministry of Labour will enforce this legal responsibility if necessary.
Employers should ensure that workers are acclimatized before they work in a hot environment. It is expected that employers would gradually increase workers’ time in hot conditions over 7 to 14 days and closely supervise new employees for the first 14 days or until they are fully acclimatized.
There are a number of points to consider:
- Non-physically fit workers require more time to fully acclimatize.
- Acclimatization can be maintained for a few days of non-heat exposure.
- Taking breaks in air conditioning will not affect acclimatization.
- If the high heat exposure is due to external temperature conditions (for example from a sudden hot day or heat wave), it is unlikely that the workers will able to adapt as the environmental conditions may not last enough to permit acclimatization.
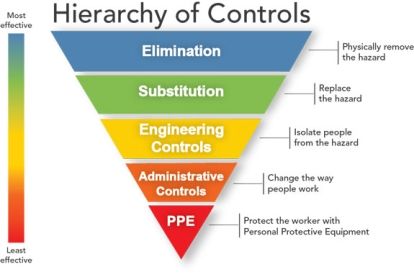
USING THE HIERARCHY OF CONTROLS FOR HEAT STRESS
Controlling exposures to occupational hazards is the fundamental method of protecting workers. The use of a hierarchy of controls is a means of determining how to implement feasible and effective control solutions. An inspection of the workplace can help determine in advance if heat is likely to be a hazard. The union and the Joint Health and Safety Committee should recommend that their employers reduce heat stress using the hierarchy of controls.
ELIMINATION
Eliminate the heat hazard by implementing air conditioning or air chilling.
SUBSTITUTION
Substitution is not applicable for heat stress.
ENGINEERING CONTROLS
- Control the heat at the source through the use of insulation and reflective barriers (insulate furnace walls).
- Exhaust hot air and steam produced by specific operations.
- Reduce the temperature and humidity through air cooling or chilling
- Provide air-conditioned rest areas.
- Increase air movement with fans if temperatures are less than 35C.
- Reduce physical demands of work task through mechanical assistance (hoists, lift-tables, etc…).
- Use reflective or heat-absorbing shielding or barriers.
- Reduce steam leaks, wet floors, or humidity.
- Allow for cooling strategies like an arm immersion cooling system. An arm immersion cooling system is a portable heat stress prevention unit that allows users to immerse their hands and forearms to reduce body heat.
ADMINISTRATIVE CONTROLS
- Implement a heat alert program whenever the weather service forecasts that a heat wave is likely to occur.
- Require workers to conduct self-monitoring and create a work group (i.e., workers, the JH&SC, a qualified healthcare provider, and a safety manager) to make decisions on self-monitoring options and standard operating procedures.
- Increase the frequency and length of rest breaks.
- Use the ACGIH TLVs for work-rest regimes, classifying all jobs as ”medium” to “heavy”.
- Schedule hot jobs to cooler times of the day.
- Provide cool drinking water near workers and remind them to drink a cup every 20 minutes or so.
- Assign additional workers or slow down the work pace.
- Make supervision “competent” in the employer’s heat stress plan, including training in the policies and procedures of the control plan
- Train workers to recognize the signs and symptoms of heat stress before hot outdoor work begins.
- Inform workers of the effects of nonoccupational factors (drugs, alcohol, obesity, etc.) on tolerance to occupational heat stress.
- Allow workers to acclimatize
- Train workers on the importance of immediately reporting to the supervisor any symptoms or signs of heat-related illness in themselves or in co-workers.
- Make workers aware of the procedures for responding to symptoms of possible heat-related illness and for contacting emergency medical services.
- implement a “Buddy System” since people are not likely to notice their own symptoms.
- Pregnant workers and workers with a medical condition should discuss working in the heat with their doctor.
PERSONAL PROTECTIVE EQUIPMENT (PPE)
PPE is the least-effective control against workplace hazards because it carries risk. PPE could be damaged, and it could give the user a false sense of security. PPE, like the kinds listed below, should always be your last line of defense against workplace hazards including heat hazards.
- Light summer clothing should be worn to allow free air movement and sweat evaporation.
- In direct sunlight, wear broad brimmed hats with neck flaps.
- Safety glasses with tinted polarized lenses should be worn outside.
- 30 SPF sun block or better.
- In a high radiant heat situation, reflective clothing may help
- Text BoxWater-cooled garments, air-cooled garments, cooling vests, bandanas and wetted overgarments
- A plastic jacket with pockets filled with dry ice or containers of ice
- Insulated gloves, insulated suits, reflective clothing and infrared reflecting face shields
- Thermally conditioned clothing, such as a garment with a self-contained air conditioner in a backpack
- A garment with a compressed air source that feeds cool air through a vortex tube
WARNING - PPE MAY INCREASE THE EFFECTS OF HEAT STRESS!
Workers are often required to wear PPE that has nothing to do with the heat and everything to do with staying safe and protected from other hazardous exposures. Vapour barrier clothing, such as acid suits, greatly increase the amount of heat stress on the body, and extra caution is necessary without even taking external heat sources into consideration. Worker exposure to chemical, biological, noise, radiation and other hazards may cause the worker to be required to wear various clothing, eye and ear protection as well as respiratory protection.
Take wearing a surgical mask for instance, during the COVID-19 pandemic, when 2m physical distancing cannot be maintained. The wearing of the mask is certainly an impediment to normal breathing and will generate additional heat on the user’s face while being worn. As the level of protection goes up on respiratory PPE (for example an N95 or better respirator), breathing resistance and additional heat will also build up on the user’s face, more than with the surgical mask. Users need to be alert to their personal circumstances and must be able to exert control of the wearing and possible removal of the PPE for the heat dissipation benefit.
When combined with other physiological problems, it is vitally important that employers take the wearing of PPE into consideration when formulating a heat stress plan. Some strategies for PPE use during hot weather include keeping PPE as cold as possible (through refrigeration) before being worn, as well as using other engineering or administrative controls in unison with cooled PPE like cooling clothing, (ice shirts, vests, neck coolers, bandanas etc.)
IN ALL CIRCUMSTANCES WHEN YOU ARE CONCERNED ABOUT YOUR HEALTH AND SAFETY, OR UNSURE OF WHAT TO DO WHEN ENCOUNTERING AN UNCONTROLLED HAZARD, DO NOT BE AFRAID TO EXERCISE YOUR RIGHTS TO KNOW ABOUT HAZARDS, TO PARTICIPATE BY RAISING CONCERNS AND BY EXERCISING YOUR RIGHT TO REFUSE UNSAFE WORK!
TIPS FOR MAINTAINING A STABLE INTERNAL CORE TEMPERATURE AT WORK
It’s better to drink small amounts frequently, as opposed to larger amounts less often, and you should drink even if you don’t feel thirsty. Avoid drinks like pop, coffee or alcoholic drinks as these drinks will dehydrate you and can make it more dangerous to work in the heat. Some people worry that if they drink a lot of water, they’ll have to go to the bathroom more often, when in fact, the excess water will mostly be released as sweat. Even when you’ve left work, you should still drink plenty of water to help your body recover from the workday.
Employers should provide the means for appropriate hydration of workers
- Water should be potable, <15°C (59°F), and made accessible near the work area.
- Estimate how much water will be needed and decide who will obtain and check on water supplies.
- Individual, not communal, drinking cups should be provided.
- Encourage workers to hydrate themselves.
Workers should drink an appropriate amount to stay hydrated
- If in the heat less than 2 hours and involved in moderate work activities, drink 1 cup (8 oz.) of water every 15–20 minutes.
- During prolonged sweating lasting several hours, drink sports drinks containing balanced electrolytes.
- Avoid alcohol and drinks with high caffeine or sugar.
- Generally, fluid intake should not exceed 6 cups per hour.
Employers should ensure and encourage workers to take appropriate rest breaks to cool down and hydrate
- Permit rest and water breaks when a worker feels heat discomfort.
- Modify work/rest periods to give the body a chance to get rid of excess heat.
- Assign new and unacclimatized workers lighter work, and longer, more frequent rest periods.
- Shorten work periods and increase rest periods:
- as temperature, humidity, and sunshine increase,
- when there is no air movement,
- if protective clothing or equipment is worn, and/or
- for heavier work.
COLLECTIVE AGREEMENTS
“There is a time and place for everything,” the old saying goes. While few employers actually agree to all excellent heat stress control recommendations made by union health and safety representatives or JH&SCs, there is a time when employers do have to “come to the table” – and that is during contract negotiation time.
Recommendations made to the employer that have been rejected during the formal JH&SC recommendation procedures in past years should be discussed with your bargaining committee and acted upon during contract negotiations. Ensure that your bargaining committee knows that heat stress language is a priority at contract time. Don’t let the employer off the hook during this fertile time to protect the membership from the dangers of heat stress. Focus on the hierarchy of controls when making heat stress related demands!
USING HEAT STRESS TOOLS FOR WORKER PROTECTION
There are a number of tools that can be used to measure the heat stress in the workplace. One of the tools is The Humidex Heat Stress Response Plan by the Occupational Health Clinics for Ontario Workers (OHCOW). It can be used when trying to do simple and objective heat stress measurements and then implement administrative controls using work/rest regimens in order to protect worker health. An explanation is available on their website: www.ohcow.on.ca
This tool uses air temperature and humidity to form a humidex-related response plan. OHCOW also has a Humidex based Heat Stress Calculator tool that aids in calculating the humidex reading and gives direction for steps to take to protect worker health.
Exposure limits intended to minimize the risk of heat-related illnesses are determined by provincial and territorial governments for most Canadian workplaces, and by Employment and Social Development Canada (ESDC) for workplaces under the federal jurisdiction. Local government labour boards or ministries of labour tend to be very conservative in their judgement of what is considered a high level of heat stress.
These agencies generally utilize the exposure guidelines recommended by the American Conference of Governmental Industrial Hygienists (ACGIH).
The ACGIH gives these exposure limits in units of WBGT (wet bulb globe temperature) degrees Celsius (°C). The WBGT unit considers environmental factors, like air temperature, humidity and air movement, which contribute to the perception of “feeling” hot. WBGT values are not at all like humidex values. In some workplace situations, the solar load (heat from radiant sources) is also considered in determining the WBGT value. Visit their website www.ccohs.ca for more information.
CONCLUSION
The workplace hazard of heat stress is one that can be both deadly and yet at the same time, easily controlled using the hierarchy of controls. In the end, each worker is different and reacts differently to this hazard. Know yourself, be in tune with your body, hydrate and watch for symptoms. Your life may depend on it! It’s better to prevent an illness than have to recuperate from one. Everyone has a role to play in keeping the workplace safe from heat stress.
Don’t be afraid to exercise your rights as workers.